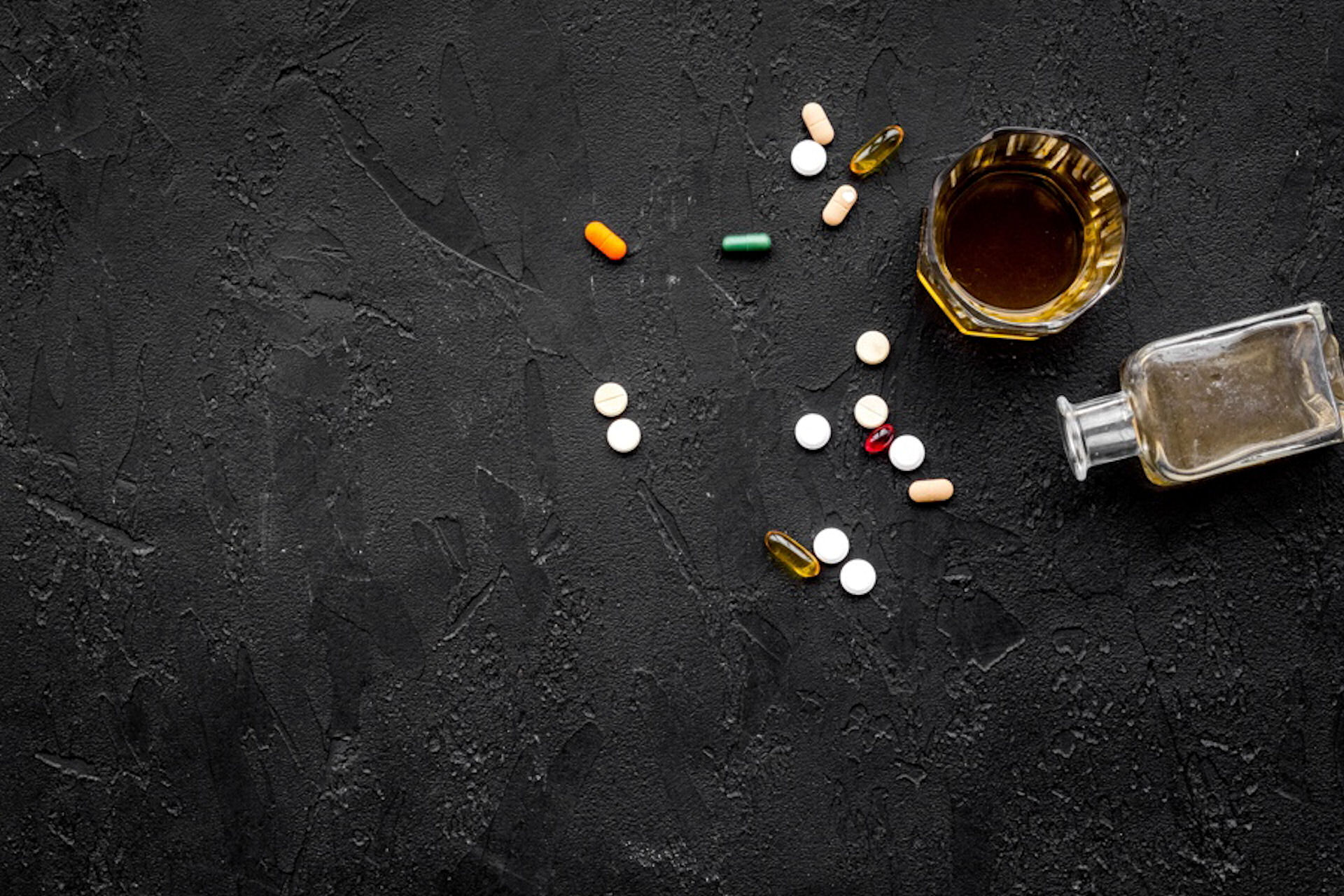
Schizophrenia and addiction are two distinct conditions, each with its own complications. When these disorders co-occur, it presents a unique challenge to healthcare professionals and adds further complexity to treatment strategies. Let’s explore the connections between schizophrenia and addiction, examining the nature of schizophrenia, how substance abuse influences it, and the potential treatment options available for these intertwined conditions.
What Is Schizophrenia and How Does It Form?

Schizophrenia is a chronic, severe mental disorder characterized by a disconnection from reality, known as psychosis. Individuals with schizophrenia may experience hallucinations, delusions, disordered thinking, and abnormal behavior, which can significantly impact daily functioning. This complex and often misunderstood condition affects approximately 1% of the global population, making it one of the most prevalent mental disorders.
The onset of schizophrenia typically occurs in late adolescence or early adulthood, with men often developing symptoms earlier than women. Although the exact cause of schizophrenia remains unknown, researchers believe that a combination of genetic, environmental, and neurochemical factors contribute to its development.
There is substantial evidence that suggests that genetics plays a strong role in the development of schizophrenia. Studies have shown that individuals with a family history of the disorder are more likely to develop it themselves. Moreover, the risk increases with the degree of genetic relatedness, meaning that the closer the biological relationship, the higher the likelihood of developing schizophrenia. However, it is important to note that genetics alone do not determine whether someone will develop the disorder. Environmental factors also play a significant role.
Various environmental factors have been linked to an increased risk of developing schizophrenia. These include prenatal exposure to infections, malnutrition, or complications during birth, as well as psychosocial factors such as childhood trauma or social isolation. Additionally, substance abuse, particularly the use of marijuana during adolescence, has been associated with an increased risk of schizophrenia. While no single environmental factor guarantees the development of the disorder, these factors can interact with genetic predispositions to increase the likelihood of developing schizophrenia.
Imbalances in brain chemicals (neurotransmitters) like dopamine and glutamate are believed to play a crucial role in the development of schizophrenia. Dopamine, a neurotransmitter responsible for regulating mood, motivation, and reward, is thought to be overactive in individuals with schizophrenia. This overactivity may contribute to the formation of delusions and hallucinations. On the other hand, an imbalance in glutamate, a neurotransmitter involved in learning and memory, has been linked to impaired cognitive functioning in people with schizophrenia.
Research has also shown that individuals with schizophrenia may have subtle differences in brain structure compared to those without the disorder. These differences include reduced gray matter volume, enlarged ventricles, and abnormal connectivity between various brain regions. Although these structural abnormalities are not present in all individuals with schizophrenia, they provide valuable insights into the potential underlying causes of the disorder.
Schizophrenia is a complex mental disorder that arises from a combination of genetic, environmental, and neurochemical factors. While researchers continue to study the precise factors that contribute to its development, understanding the specifics can help inform prevention strategies and treatment options for those affected by this overwhelming condition. With ongoing research and increased awareness, there is hope for improved outcomes and a better quality of life for those living with schizophrenia.
Substance abuse can significantly exacerbate the symptoms of schizophrenia. Certain substances, such as cannabis, stimulants, and alcohol, can induce psychosis and potentially trigger a schizophrenic episode in vulnerable individuals. Moreover, substance use can interfere with the effectiveness of antipsychotic medications, often leading to poorer treatment outcomes.
Individuals with schizophrenia are much more likely to develop a substance use disorder compared to the general population. This co-occurrence can be partly attributed to self-medication theory, suggesting that people with schizophrenia may use substances to cope with distressing symptoms or side effects of medication. However, this often results in a vicious cycle, as substance use worsens symptoms and can lead to more frequent and severe psychotic episodes.
While the precise cause of schizophrenia is unknown, certain risk factors are associated with its development. These include genetic predisposition, brain chemistry imbalances, certain viral infections during prenatal development, and psychosocial factors like stressful environments and trauma. Substance use is also a potential risk factor, particularly during adolescence when the brain is still developing.
Signs and Symptoms Associated with Schizophrenia and Addiction
Schizophrenia is a mental health problem that causes people to have trouble with reality. It has three types of symptoms: positive, negative, and cognitive.
Positive symptoms:
- Hallucinations: Hearing or seeing things that aren’t real
- Delusions: Believing things that aren’t true
- Disorganized speech: Talking in a way that doesn’t make sense
- Disorganized behavior: Acting strange or unpredictable
Negative symptoms:
- Apathy: Not caring about daily activities
- Anhedonia: Not being able to feel happy or enjoy things
- Social withdrawal: Avoiding other people
- Flat affect: Not showing emotions
Cognitive symptoms:
- The trouble with memory: Forgetting things easily
- Attention problems: Not being able to focus well
- The trouble with problem-solving, planning, and organizing
Addiction is when someone can’t stop using a substance, like drugs or alcohol, even if it causes harm. Some signs of addiction are:
- Using the substance even when it’s harmful
- Strong cravings for the substance
- Needing more of the substance to feel the same effects
- Feeling sick or uncomfortable when not using the substance
Challenges in Knowing if Someone Has Both Schizophrenia and Addiction
When someone has both schizophrenia and addiction, it can be hard to tell which symptoms come from each problem. This can make it difficult to figure out the right treatment. Some challenges include:
- Figuring out if the symptoms are because of schizophrenia, addiction, or both
- Telling the difference between drug-induced psychosis and schizophrenia
- Understanding how severe each problem is and how they affect daily life
- Finding the right treatment for both problems
By knowing the signs of schizophrenia and addiction, doctors can better help people with these issues. Getting help early and having a treatment plan that covers both problems can make a big difference in a person’s life.
Treatment Options for Schizophrenia and Addiction

Treating co-occurring schizophrenia and addiction necessitates a comprehensive, integrated approach that addresses both conditions simultaneously.
Antipsychotic medications form the cornerstone of schizophrenia treatment, helping to control symptoms by affecting dopamine and other neurotransmitters. Psychotherapy, including individual and group therapy, and social skills training, are also integral components.
Treatment for addiction typically involves detox, behavioral therapy (such as cognitive-behavioral therapy and motivational interviewing), and support groups. In many cases, the individual will likely need to enroll in an inpatient or outpatient treatment program in order to better understand how to manage symptoms related to these disorders.
Importance of Dual Diagnosis Treatment
Dual diagnosis treatment is vital when it comes to treating schizophrenia and addiction. This approach recognizes the interplay between these conditions and ensures that treatment targets both simultaneously. By neglecting one condition, we risk exacerbating the other, leading to a cycle of worsening mental health and escalating substance use.
Our Approach to Treatment at Westwind Recovery®®
At Westwind Recovery®®, we understand the intricacies of dual diagnosis treatment. Our approach emphasizes the importance of understanding the interconnected nature of schizophrenia and addiction. We use evidence-based treatment strategies designed to address the whole person, not just their disorders.
These strategies include medication-assisted treatment, where medications are used to manage symptoms of schizophrenia and to aid in addiction recovery. The therapeutic component of the treatment involves different modalities such as cognitive-behavioral therapy, dialectical behavior therapy, and motivational interviewing. These therapies are tailored to help individuals understand their conditions, develop healthier coping mechanisms, and work towards their recovery goals.
In addition to this, we provide a nurturing, supportive community, echoing our belief that recovery is most successful when tackled as a team effort. We offer peer support groups where individuals can share their experiences, challenges, and successes, fostering a sense of belonging and mutual understanding.
Furthermore, we understand the importance of family involvement in the recovery process. Family therapy sessions are incorporated into our treatment programs, allowing families to better understand their loved one’s conditions and learn how they can support them in their recovery journey.
Finally, we emphasize the importance of aftercare and ongoing support following the completion of treatment. This can involve continued outpatient therapy, participation in self-help groups, and ongoing medication management.
Do You Have More Questions About Schizophrenia and Drug Use?
Schizophrenia and addiction can, unfortunately, form a harmful synergy, each condition feeding into the other and leading to worsened outcomes. However, with an integrated, comprehensive approach, recovery is not only possible but expected.
With the right support, individuals can manage their symptoms, overcome addiction, and lead fulfilling, healthier lives. The road to recovery may be challenging, but with the right care and support, it can also be a journey of self-discovery, personal growth, and renewed hope. At Westwind Recovery®®, we’re here to provide that care and support every step of the way.

Dr. Deena is the Chief Clinical Officer of Westwind Recovery®, an award-winning outpatient treatment center in Los Angeles where she oversees the clinical and administrative program and treatment methods. Dr. Deena is a doctor of psychology and licensed clinical social worker since 1993. LCSW #20628. Originally from the East Coast, Dr. Deena has worked running treatment centers, worked as a therapist in psychiatric hospitals as well as school settings and currently has a thriving private practice in the LA area. Dr. Deena has appeared regularly on the Dr. Phil Show as an expert since 2003. She has also been featured on many other TV shows, podcasts and has contributed to written publications as well as podcasts.